Latest News

Flag-raising ceremonies honor lifesaving organ donation
Penn State Health honored organ donors and recipients and raised awareness for organ donation at an event on the Milton S. Hershey Medical Center and Holy Spirit Medical Center campuses.
Read MoreTwo College of Medicine graduate students receive prestigious Penn State awards
Two graduate students at Penn State College of Medicine have received the prestigious Penn State Alumni Association Dissertation Award.
Read MorePreventing child abuse: How parents can keep their children safe
April is National Child Abuse Prevention Month. Get some tips on what you can do to keep your children safe.
Read MorePenn State Health celebrates 40th anniversary milestone in heart transplant care
Milton S. Hershey Medical Center celebrated its 40th anniversary of providing heart transplants to patients in the region with a special event for its multidisciplinary heart transplant team on Feb. 22.
Read MorePenn State Health celebrates Donate Life Month with flag-raising, Blue & Green Day
Penn State Health will honor organ donors and highlight the increasing need for organ donations with two events during National Donate Life Month in April.
Read MoreLatest Research
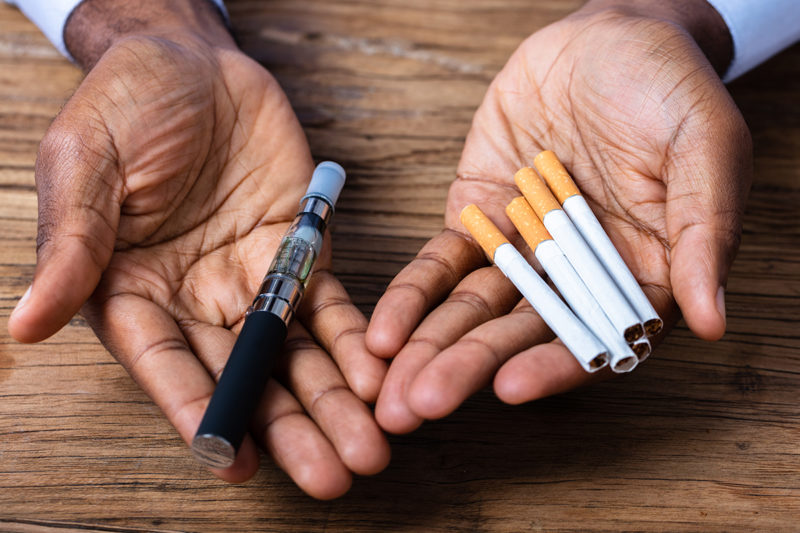
College of Medicine receives $20M grant to research alternative tobacco products
Penn State College of Medicine received a five-year, $20 million federal grant to investigate the harmful effects of alternative tobacco products.
Read MorePenn State's Project ECHO team attends MetaECHO global conference
In 2023 Project ECHO celebrated its 20th anniversary along with the return of its annual conference, MetaECHO. The institute’s first gathering since 2019, MetaECHO 2023 was held in Albuquerque, New […]
Read MoreDonors continue son’s legacy with estate gift to personalized medicine
A recent estate gift from Dr. and Mrs. Vali and Pari Kermani will expand the Kia Kermani Foundation Research Fund for Personalized Medicine at Penn State College of Medicine.
Read MoreAdvanced imaging gives researchers front row view of cellular junctions
Penn State College of Medicine researchers used focused ion beam scanning electron microscopy to reveal a previously unknown complex formed at cell-to-cell junctions consisting of desmosomes, keratin filaments and endoplasmic reticulum.
Read MoreRh sensitization treatment may be unnecessary in first trimester pregnancies
An immune treatment may not be necessary until after the first trimester of pregnancy, according to Penn State research. The results could change pregnancy care guidelines and close health equity gaps.
Read MoreLatest Medical Minutes
The Medical Minute: Six organ donation facts knock down six myths
More than 103,000 people in the U.S. are awaiting new organs. Many won’t live long enough to get them. The new chief of transplant at Penn State Health Milton S. Hershey Medical Center debunks the myths that get between donors and recipients.
Read MoreThe Medical Minute: April fools vs. April facts
‘Tis the season of April trickery. Five Penn State health experts help you separate what’s real and what’s myth.
Read MoreThe Medical Minute: Help your children experience the solar eclipse while protecting their vision
It’s a celestial anomaly that happens only once in a blue moon. A Penn State Health expert talks about the safest ways for you to witness the solar eclipse on Monday, April 8.
Read MoreThe Medical Minute: Vitamin supplements versus a balanced diet? No contest
The use of vitamin supplements is on the rise in the U.S. But do they do any good? A Penn State Health expert talks about the benefits and pitfalls.
Read MoreThe Medical Minute: Colon cancer rates higher in rural areas
Technology to stop or prevent colon cancer keeps improving. Still, incident rates remain more stubborn in rural areas than urban centers. The dean of Penn State College of Medicine talks about the barriers.
Read MoreLatest Education

Hackman and Bonaddio recognized for Exceptional Moments in Teaching
Nicole Hackman, MD, faculty member, and Vincenzo Bonaddio, MD, resident, were recognized through the “Exceptional Moments in Teaching” program for April.
Read MoreThompson and Sallam recognized for Exceptional Moments in Teaching
Andrew Thompson, MD, and Eman Sallam, MD, were recognized through the “Exceptional Moments in Teaching” program for March.
Read MoreHenao and O’Bryant recognized for Exceptional Moments in Teaching
Maria Paula Henao, MD, faculty member, and Michael O’Bryant, DO, resident, are the February awardees through the “Exceptional Moments in Teaching” program.
Read MoreGrogan and Eng recognized for Exceptional Moments in Teaching
James Grogan, MD, faculty member, and Nina Eng, MD, resident, were recognized through the “Exceptional Moments in Teaching” program for the month of January.
Read MoreHess and Bavier recognized for Exceptional Moments in Teaching
Stacy Hess, MD, faculty member, and Richard Bavier, MD, resident, were recognized through the “Exceptional Moments in Teaching” program for the month of November.
Read MoreLatest Patient Care

Behind Every ER Visit: The Essential Role of Patient Registration Associates at Penn State Health
A trip to the emergency room is something no one wants to experience. People arrive by ambulance and by car, hurting and scared. Fast, quality care is essential—but so is […]
Read MoreDiabetes disparities: Penn State Health diabetes specialist works to improve health equity
No one wants to hear the “Big D” diagnosis—diabetes. If you’re a person of color, diabetes management may be affected by limited access to technology, increasing risk of complications.
Read MoreMilton S. Hershey Medical Center’s heart transplant survival rate highest in the state
More than 94 percent of all patients who receive a heart transplant at Penn State Health Milton S. Hershey Medical Center survive for at least three years after their surgery.
Read MoreBreakthrough stroke treatment at Penn State Health offers patients new hope
The Vivistim Paired VNS (vagus nerve stimulation) System pairs a surgically implanted device with physical or occupational therapy for people who have moderate to severe upper arm impairment following a stoke.
Read MoreChildren's Hospital earns Parent Project Muscular Dystrophy certification
Parent Project Muscular Dystrophy has certified the clinic at Penn State Health Children's Hospital.
Read MoreLatest Ask Us Anything About

Ask Us Anything About… Enlarged Prostates
There are more treatment options than ever for enlarged prostate, according to Dr. Jaime Herrera Caceres, a urologist at Penn State Health's Hampden Medical Center and Holy Spirit Medical Center.
Read MoreAsk Us Anything About… Stomach Pain
We all have stomach pains from time to time. But how can we pinpoint the cause and determine when it may be serious and warrant medical attention?
Read MoreAsk Us Anything About… Cholesterol Screening
Dr. Patrick Fitzsimmons, an interventional cardiologist at Penn State Health Lancaster Medical Center, covers what you need to know about cholesterol and the importance of knowing your numbers.
Read MoreAsk Us Anything About… RSV in Children
We’ve been hearing a lot about RSV -- or respiratory syncytial virus -- lately. While cases are reported every year, an early influx of cases -- and of hospitalizations, including among children -- is adding to concern this year. We find out what parents need to know from Dr. Jessica Ericson, a pediatric infectious diseases physician, and Dr. Duane Williams, a pediatric critical care physician -- both of Penn State Health Children's Hospital.
Read MoreAsk Us Anything About... Knee Problems
Approximately a quarter of all adults suffer from knee pain. We learn more about the causes of and treatments for a range of knee ailments from two Penn State Health orthopedic surgeons: Dr. Charles Davis and Dr. Aman Dhawan.
Read MoreLatest Community

April 27 | Dispose of medications safely on National Prescription Drug Take-Back Day
Penn State Health will collect unwanted, unneeded or expired medication for safe disposal on Saturday, April 27, as part of the U.S. Drug Enforcement Administration National Prescription Drug Take-Back Day.
Read MorePenn State Health diabetes specialist: Make ‘personal choice’ to address health equity
Deciding to take the journey is as important as the journey. That’s how a Penn State Health diabetes educator characterizes efforts to learn how technology access affects outcomes for minorities.
Read MoreEducation on religious observances helps Penn State Health promote quality patient experience
Easter, Ramadan and Passover are underway or will take place soon. Penn State Health has educated employees on respecting requests they may receive from people who observe the holidays.
Read MorePenn State Health honors trailblazers during Black History Month
During Black History Month, Penn State Health honors and celebrates the contributions of some of its trailblazers who have left on their marks on society and advocate for equality, justice and progress.
Read MoreAngels of Lancaster: Penn State Health community nurse addresses health inequities person by person
Angela Shuman is a conduit to health care for people who need it desperately, but can’t always access it.
Read MoreLatest People
![[2:12 PM] McVitty, Vanessa stephens-1200x800.png Caption: Heather Stephens, a neonatal clinical nurse specialist at Milton S. Hershey Medical Center Alt Text: Portrait of lady wearing suit jacket over a patterned shirt, smiling. The portrait is overlaid on an image of a Nittany Lion statue.](https://pennstatehealthnews.org/wp-content/uploads/2024/04/stephens-1200x800-1-800x533.png)
Advanced Practice Provider Spotlight: Neonatal clinical nurse specialist explores how diversity and language services improve patient care
Neonatal clinical nurse specialist Heather Stephens highlights the critical need for more diversity among advanced practice providers to serve the increasingly diverse patient population.
Read MoreAdvanced Practice Provider Spotlight: Nurse midwife shares insights on caring for diverse patients
After receiving care from midwives during the birth of her son, Jennifer Pagani-Smith said she felt “called” to become a certified nurse midwife and help empower other women.
Read MoreHershey Medical Center honors DAISY Award winners, Haas, Nye, Strine
Hershey Medical Center presented its quarterly DAISY (Diseases Attacking the Immune System) Award for Extraordinary Nurses to Jess Haas, Marissa Nye, and Theresa Strine.
Read MoreMilton S. Hershey Medical Center names Harbaugh chief medical officer
Milton S. Hershey Medical Center appointed Dr. Robert Harbaugh to the position of chief medical officer.
Read MorePenn State Health appoints Leslyn Williamson chief operating officer for Hampden and Holy Spirit medical centers
Leslyn Williamson has been named chief operating officer for Penn State Health Hampden Medical Center and Penn State Health Holy Spirit Medical Center. She will continue as the chief nursing officer for both hospitals.
Read More




